Living with diabetes doesn’t mean giving up an active lifestyle. In fact, exercise is one of the most powerful tools you have for managing blood sugar levels. But it’s not as simple as just moving more. Understanding how physical activity affects your glucose, when to exercise, and how to stay safe makes all the difference between a beneficial workout and a potentially dangerous situation.
This guide will walk you through everything you need to know about exercising safely with diabetes, from choosing the right activities to monitoring your blood sugar and recognizing warning signs.
How Different Types of Exercise Affect Your Blood Sugar
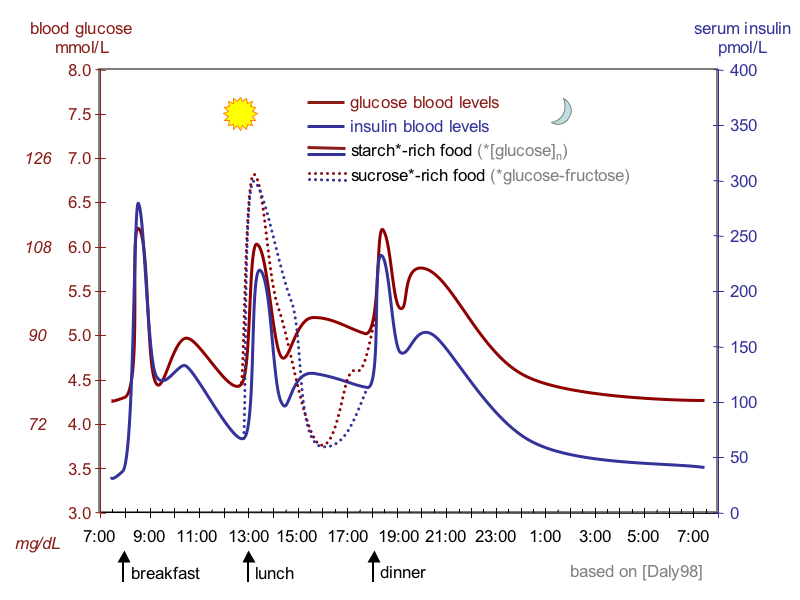
Not all exercise impacts your glucose the same way. Aerobic activities like walking, swimming, and cycling typically lower blood sugar both during and after your workout. Your muscles use glucose for fuel, which pulls sugar out of your bloodstream and can continue doing so for up to 24 hours after you finish.
Resistance training works differently. Lifting weights or using resistance bands can actually cause a temporary spike in blood sugar during your workout due to stress hormones. However, within a few hours, your levels typically drop as your muscles repair and rebuild. Over time, strength training improves insulin sensitivity, making it easier for your body to regulate glucose.
High-intensity interval training (HIIT) can be tricky. Short bursts of intense activity may raise blood sugar initially, then cause it to drop hours later. This delayed effect is why monitoring becomes especially important with vigorous exercise.
The best approach combines both aerobic and resistance training. Aim for at least 150 minutes of moderate aerobic activity per week, plus two to three strength training sessions. Start slowly and build up gradually if you’re new to exercise.
Timing Your Exercise Around Meals and Medication

When you exercise matters just as much as what you do. For most people with diabetes, the ideal window is one to three hours after eating. Your blood sugar is elevated from the meal, reducing the risk of hypoglycemia during activity.
Exercising on an empty stomach or when your last meal was more than four hours ago increases your risk of low blood sugar, especially if you take insulin or certain oral medications. If you prefer morning workouts before breakfast, have a small snack with 15-20 grams of carbohydrates about 30 minutes beforehand.
Medication timing requires careful coordination. If you take rapid-acting insulin with meals, waiting 90 minutes to two hours before exercising allows the insulin peak to pass. For those on long-acting insulin, consistency is key. Exercise at roughly the same time each day so you and your healthcare provider can adjust your doses if needed.
Keep a log of your blood sugar readings before and after exercise, along with notes about what and when you ate. Patterns will emerge that help you fine-tune your routine. A reliable blood glucose monitor makes this tracking much easier.

Contour Next EZ Blood Glucose Monitor
Highly accurate and easy to use, perfect for checking levels before and after workouts.
Recognizing and Responding to Blood Sugar Changes During Activity
Hypoglycemia (low blood sugar below 70 mg/dL) is the most common concern during exercise. Early warning signs include shakiness, sweating, dizziness, confusion, rapid heartbeat, and sudden fatigue. Some people experience irritability or anxiety.
Stop exercising immediately if you notice any of these symptoms. Check your blood sugar right away. If it’s below 70 mg/dL, follow the 15-15 rule: consume 15 grams of fast-acting carbohydrates, wait 15 minutes, then test again. Repeat if necessary.
Good options for treating lows include glucose tablets, half a cup of juice, or regular soda. Always carry these with you during exercise. Glucose tablets are particularly convenient because they’re measured and portable.
Hyperglycemia (high blood sugar above 250 mg/dL) also deserves attention. If your blood sugar is this high before exercise, check for ketones. The presence of ketones means you should skip your workout and contact your healthcare provider. Exercise with ketones present can make the situation worse.
Without ketones, light to moderate exercise may actually help lower elevated glucose. Avoid intense workouts when your blood sugar is high, as these can trigger an additional spike.
Creating Your Safe Exercise Routine
Start by getting medical clearance from your doctor, especially if you’ve been inactive or have diabetes complications. They may recommend specific tests to check your heart, eyes, kidneys, and nerves before you begin a new program.
Build your routine gradually. Begin with just 10-15 minutes of activity and add five minutes each week until you reach your goal. This prevents overexertion and allows you to observe how different durations affect your blood sugar. Regular physical activity delivers numerous health benefits beyond blood sugar control, including improved cardiovascular health and better mobility.
Choose activities you enjoy. You’re much more likely to stick with dancing, gardening, or playing with grandchildren than forcing yourself through a dreaded treadmill session. The best exercise is the one you’ll actually do consistently. Even everyday activities like building functional strength through carrying groceries can contribute to better diabetes management.
Consider exercising with a partner who knows you have diabetes and understands what to do if problems arise. Wear a medical ID bracelet that indicates you have diabetes. In an emergency, this information could be lifesaving.
Proper footwear matters tremendously for people with diabetes. Neuropathy can reduce sensation in your feet, making blisters and injuries easy to miss. Invest in well-fitting athletic shoes designed for your chosen activity and check your feet daily for any signs of trouble.

New Balance 928v3 Walking Shoes
Excellent support and cushioning for daily walks, with a design that accommodates diabetic foot concerns.
Blood Sugar Monitoring Guidelines
Check your blood sugar before every workout. If it’s below 100 mg/dL, have a small snack before starting. Between 100-250 mg/dL without ketones is generally safe for exercise. Above 250 mg/dL, check for ketones and proceed cautiously or skip the workout based on the results.
During extended exercise sessions lasting more than 60 minutes, check your levels every 30-45 minutes. This is particularly important when you’re first establishing your routine and learning how your body responds.
Always test again 15-30 minutes after finishing your workout. This helps you catch any delayed drops in blood sugar. For some people, glucose levels continue falling for several hours post-exercise, so additional checks before bed may be necessary if you exercised in the evening.
Continuous glucose monitors (CGMs) have changed the game for active people with diabetes. These devices track your levels throughout the day and night, alerting you to trends before problems develop. Many CGM supplies and accessories are available to help you manage the technology during workouts.
When to Contact Your Healthcare Provider
Certain situations require professional guidance rather than self-management. Reach out to your doctor if you experience frequent low blood sugar during or after exercise despite adjusting your routine and carbohydrate intake.
Persistent high blood sugar that doesn’t respond to your usual interventions also warrants a call. Your medication doses may need adjustment to account for your new activity level.
Contact your healthcare team if you develop new symptoms during exercise like chest pain, severe shortness of breath, vision changes, or numbness and tingling in your extremities. These could indicate complications that need evaluation.
Schedule regular check-ins even when things are going well. Your doctor should review your blood sugar logs, adjust medications as needed, and help you progress safely toward your fitness goals. Most healthcare providers love seeing patients take an active role in managing their diabetes through exercise.
Frequently Asked Questions
Can I exercise if my diabetes isn’t well controlled?
You can still be active, but you’ll need to work closely with your healthcare team first. Start with gentle activities like short walks and monitor your blood sugar carefully. Avoid intense exercise until your glucose levels are more stable. Getting your diabetes under better control should be the priority, and moderate activity can actually help with that goal.
How long after starting an exercise program will I see improvements in my blood sugar?
Many people notice immediate effects, with lower blood sugar during and after individual workout sessions. Long-term improvements in insulin sensitivity typically show up within two to four weeks of regular activity. You may see your A1C numbers improve within two to three months. Keep in mind that consistency matters more than intensity when it comes to sustained benefits.
What should I keep in my exercise bag for diabetes management?
Pack your blood glucose meter and extra test strips, glucose tablets or another fast-acting carbohydrate source, a bottle of water, and a small protein-carb snack for after your workout. Include your medical ID information and emergency contact numbers. If you use insulin, bring your supplies and know how to adjust doses based on your activity. A small towel and extra socks can prevent blisters and discomfort during longer sessions.
Related Articles
- Building Functional Strength for Carrying Groceries as a Senior
- Benefits of Resistance Training for Seniors Over 65
- 8 Health Benefits of Fig Leaves: Boost Digestion, Heart Health & More Naturally
- Unlocking the Power of Fitness: Top Health Benefits for Seniors
This article contains affiliate links. We may earn a small commission at no extra cost to you.
