You’ve committed to staying active in your senior years, and that’s fantastic. Regular exercise can help you maintain independence, manage chronic conditions, and improve your quality of life. But if you’re taking medications for blood pressure, diabetes, or heart conditions, timing matters more than you might realize.
The interaction between your medications and your workout schedule isn’t just about avoiding discomfort. It can affect how well your medications work, how your body responds to exercise, and your overall safety during physical activity. Understanding these interactions helps you get the most benefit from both your medications and your exercise routine.
How Blood Pressure Medications Affect Your Exercise Timing
Blood pressure medications work in different ways, and each type has its own considerations when it comes to exercise timing. Beta-blockers like metoprolol and atenolol slow your heart rate, which means you can’t use your usual heart rate zones to gauge exercise intensity. These medications also peak in your bloodstream about 2 to 4 hours after you take them.
Many seniors find that exercising right when beta-blockers are at their peak can leave them feeling unusually tired or dizzy. Your blood pressure drops during this window, and adding exercise can amplify that effect. You might want to schedule your workouts for later in the day if you take your beta-blocker in the morning, or talk to your doctor about splitting your dose.
Diuretics, often called water pills, present a different challenge. Furosemide and hydrochlorothiazide make you urinate more frequently, especially in the first few hours after taking them. Plan your exercise for later in the day if you take diuretics in the morning, or you’ll spend half your workout time looking for a bathroom. More importantly, diuretics can lead to dehydration and electrolyte imbalances during exercise.
ACE inhibitors like lisinopril and calcium channel blockers like amlodipine tend to be more forgiving with exercise timing. They work more steadily throughout the day. Still, you should avoid exercising during the first hour after taking them, when absorption is happening and side effects like dizziness are more likely.
Managing Diabetes Medications Around Your Workout
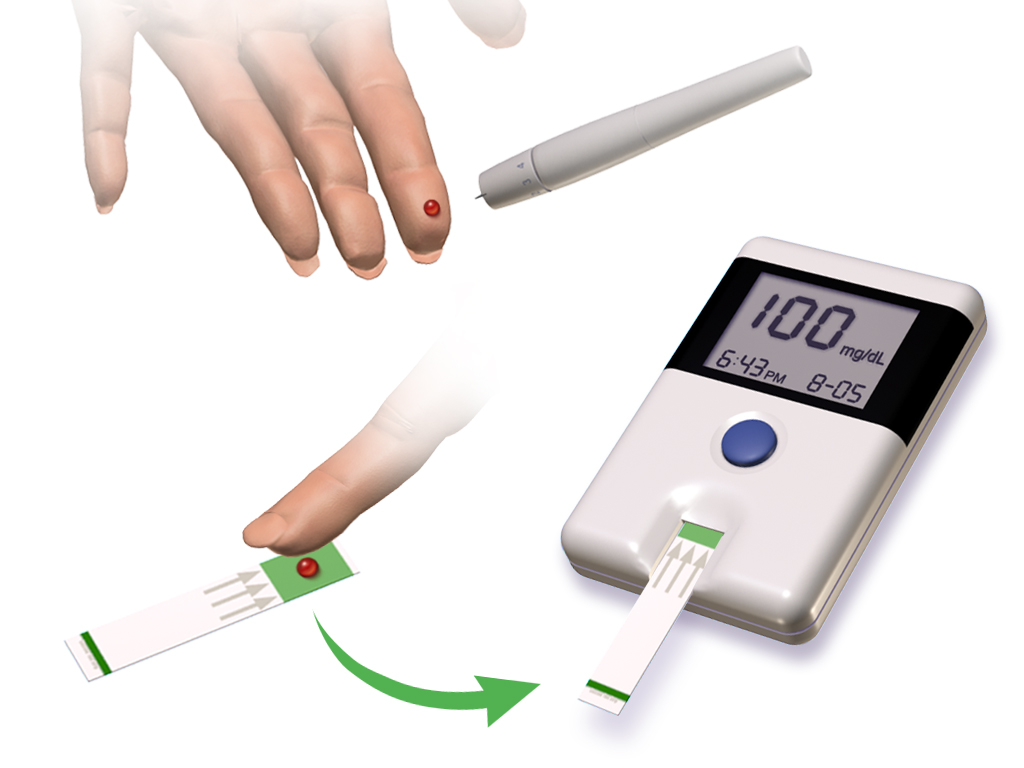
Blausen.com staff (2014). “Medical gallery of Blausen Medical 2014”. WikiJournal of Medicine 1 (2). DOI:10.15347/wjm/2014.010. ISSN 2002-4436., CC BY 3.0, via Wikimedia Commons
Diabetes medications require the most careful attention to timing because exercise itself lowers blood sugar. When you combine that effect with medication, you risk dangerous hypoglycemia. This is particularly true if you’re taking insulin or sulfonylureas like glyburide or glipizide.
For insulin users, the timing gets complicated because different types peak at different times. Rapid-acting insulin peaks in 1 to 2 hours, short-acting in 2 to 4 hours, and intermediate-acting in 4 to 12 hours. Exercising during these peak times significantly increases your risk of low blood sugar. You’ll need to check your glucose before, during, and after exercise, and you might need to reduce your insulin dose or eat extra carbohydrates.
Metformin, the most commonly prescribed diabetes medication, doesn’t typically cause low blood sugar on its own. However, exercising in hot weather while taking metformin can increase your risk of lactic acidosis, a rare but serious condition. Stay well-hydrated and avoid intense exercise in extreme heat.
If you’re on newer medications like SGLT2 inhibitors (such as empagliflozin) or GLP-1 agonists (like semaglutide), you have a bit more flexibility. These medications work differently and carry lower hypoglycemia risk. You still need to monitor your blood sugar, but you won’t need to time your exercise as precisely around your medication schedule.
Heart Medications and Exercise Considerations

Heart medications deserve special attention because they directly affect how your cardiovascular system responds to physical stress. If you’re taking nitrates for angina, like nitroglycerin or isosorbide, you need to understand that exercise itself dilates blood vessels. Combining that with nitrates can cause severe drops in blood pressure.
Take your nitrates as prescribed before exercise if your doctor has recommended that approach for preventing exercise-induced angina. Just be aware that you might feel lightheaded when you start moving. Warm up very gradually and have a plan for sitting down quickly if needed.
Anticoagulants like warfarin, apixaban, or rivaroxaban don’t directly affect your exercise capacity, but they do increase bleeding risk. Activities with fall risk or contact become more dangerous. This doesn’t mean you should avoid exercise, but you might want to schedule higher-risk activities when your medication levels are lowest, typically right before your next dose.
Digoxin, used for heart failure and atrial fibrillation, has a narrow therapeutic window. Dehydration and electrolyte changes from exercise can push you into toxic levels. Keep your exercise moderate, stay well-hydrated, and watch for signs of digoxin toxicity like nausea, visual changes, or irregular heartbeat.
Recognizing Medication-Exercise Interactions
Your body will usually tell you when something isn’t right, but you need to know what to watch for. Unusual fatigue that’s different from normal exercise tiredness often signals a problem. You should feel tired after a workout, but if you’re exhausted after minimal activity, your medication timing might need adjustment.
Dizziness or lightheadedness, especially when standing up or changing positions during exercise, suggests your blood pressure is dropping too low. This commonly happens when blood pressure medications peak at the same time you’re exercising. Stop what you’re doing, sit down, and check your blood pressure if possible.
Rapid or irregular heartbeat during exercise that feels different from your normal response deserves immediate attention. Some medications affect heart rhythm, and exercise can amplify these effects. Learn what your typical heart rate pattern feels like during exercise so you can recognize when something changes.
Shakiness, confusion, sweating, or sudden hunger during exercise are classic signs of low blood sugar. If you’re on diabetes medications, you should always have fast-acting carbohydrates with you during exercise. Glucose tablets work best, but fruit juice or regular soda will do in a pinch.
Muscle cramps or weakness that’s more severe than usual might indicate electrolyte imbalances, particularly if you’re on diuretics. This isn’t just uncomfortable; it can affect your heart rhythm and increase fall risk.
Creating Your Personal Exercise and Medication Schedule
Start by making a detailed list of all your medications, including the time you take each one and when it reaches peak levels. Your pharmacist can provide peak time information for each medication. Map this out visually so you can see the windows where multiple medications might be at their highest levels.
Look for gaps in your medication schedule where you have the fewest overlapping peak times. These are your best exercise windows. For many seniors taking morning medications, this sweet spot falls in the late afternoon or early evening. Your medications have mostly leveled out, but you haven’t taken evening doses yet.
Test your chosen exercise time for at least two weeks before committing to it. Keep notes about how you feel before, during, and after exercise. Track your blood pressure and blood sugar if relevant. This data helps you and your healthcare provider fine-tune the timing.
Consider splitting your exercise into shorter sessions if your medication schedule is complex. Two 15-minute walks might work better than one 30-minute session, allowing you to work around multiple medication peak times. Shorter sessions also reduce the overall stress on your system.
Safety Guidelines You Can’t Ignore
Never adjust your medication timing or dosage without talking to your doctor first. Even if you think a change would help your exercise routine, medications are prescribed on specific schedules for good reasons. Your doctor can help you find solutions that don’t compromise your treatment.
Always carry identification that lists your medications when you exercise, especially if you exercise away from home. A medical ID bracelet or a card in your wallet can be lifesaving if you have a medical emergency during exercise. First responders need to know what medications you’re on.
Keep your emergency contacts and your doctor’s number in your phone and tell someone where you’ll be exercising. This applies whether you’re walking around your neighborhood or using a gym. Solo exercise is fine, but someone should know your plans.
Invest in a reliable blood pressure monitor and blood glucose meter if you’re on medications that require monitoring. Check your levels before exercise, and know your personal thresholds for when it’s safe to exercise and when you need to skip it. Generally, blood pressure above 180/110 or below 90/60, or blood sugar below 100 or above 250 mg/dL means you should postpone exercise.
Stay well-hydrated, but don’t overdo it. Excessive water intake can dilute your electrolytes, which is particularly problematic if you’re on diuretics. Sip water regularly throughout exercise rather than gulping large amounts at once.
Working With Your Healthcare Team
Your primary care doctor should know about your exercise plans, but don’t stop there. Your cardiologist, endocrinologist, or other specialists have valuable input about how your specific conditions and medications interact with physical activity. Bring your exercise schedule to your appointments and ask specifically about timing concerns.
Pharmacists are underused resources for medication timing questions. They often have more time than your doctor to discuss the practical aspects of taking medications around your daily activities. Ask your pharmacist about the best time to take each medication relative to exercise, meals, and your other medications.
Consider working with a physical therapist or exercise physiologist who has experience with seniors on multiple medications. They can design a program that accounts for your medication schedule and teach you how to monitor yourself during exercise. Many insurance plans cover these services with a doctor’s referral.
Schedule a medication review at least annually, or whenever you start a new medication or change your exercise routine. Your needs change over time, and what worked last year might not be optimal now. Regular reviews help catch potential problems before they become serious.
Frequently Asked Questions
Can I exercise on an empty stomach if I take morning medications?
This depends on your specific medications. Some medications work better on an empty stomach, while others need food to prevent stomach upset. More importantly, exercising on an empty stomach while taking diabetes medications can be dangerous. Talk to your doctor about your specific situation, but generally, having a small snack before morning exercise is safer for most seniors on multiple medications.
What should I do if I forget to take my medication before my scheduled exercise time?
Don’t skip your medication or take it right before exercise to catch up. Take it as soon as you remember and adjust your exercise timing accordingly. If it’s close to your next scheduled dose, call your pharmacist for guidance. Missing one exercise session is better than risking a medication interaction or inadequate disease control.
How long should I wait after taking medication before I start exercising?
This varies by medication type. Generally, waiting at least 30 to 60 minutes after taking any medication gives your body time to start absorbing it and reduces immediate side effects. For blood pressure medications, waiting 2 to 3 hours helps you avoid exercising during peak drug levels. Your pharmacist can give you specific timing for each of your medications.
Is it safe to exercise if I feel fine but my numbers are slightly out of range?
Don’t exercise based on how you feel alone. Slightly elevated blood pressure or blood sugar might not cause symptoms but can still be dangerous during exercise. Follow the guidelines your doctor has given you for safe exercise ranges. If your numbers are consistently out of range, you need to talk to your doctor about adjusting your medications rather than exercising when it’s not safe.

